Wednesday 25 January 2012 was just like any other day, I got up, went to work, I can’t remember what the weather or what I was wearing, come to think of it I don’t remember much about the days/weeks leading up to it.
But I do know it was my lucky day.
Lucky Day

My first memories following that day are of gradually waking up in the hospital about two weeks later to the sound of beeping machines. I remember feeling terrified, wondering what had happened and trying to express the fear with my eyes, which must have looked very odd, I could not talk because I had a tracheotomy.
As I woke I recognised my husband and two daughters who had been at my bedside the whole time, along with the doctors and nurses they began to tell me about my fight for life a little bit at a time.
Apparently, I had been sitting on the church wall outside my place of work talking to my daughter Hayley who had come to meet me at lunchtime to tell me how her first day on a university course had gone.
None of this I remember but I was told I had had a sudden cardiac arrest.
Clair my other daughter said she had thought I had been looking rather grey and tired of late, with hindsight I remember having some hot flushes, palpitations and feeling very tired. Which I dismissed as being a part of my age and menopausal symptoms, I remember thinking “oh just get on with it Susan”.
My collapse was very sudden.
As my daughter and I sat chatting I said that I felt funny. With a massive thud, I hit the ground, in what looked like a type of seizure. I hit my head and chest on the hard cobbles, cracking my cheekbone and put my teeth through my bottom lip. Hayley ran into my work and asked staff to phone for an ambulance and returned to me. As she bent over me to wipe the blood away I stopped breathing, then the first responders arrived. The paramedic later told me that, my heart was flickering erratically, in what is known as ventricular fibrillation, which cannot sustain life.
I was dead!
However, this turned out to be my lucky day.
Dead?

First responders and paramedics were at my side within less than three minutes, because at that time they were based on the car park nearby. They cleared my airway of blood and gave me the all-important CPR and defibrillation.
I’m not sure how many shock treatments I had, but they managed to put in a tube to protect my airway and a cannula in my arm while continuing CPR during the short ride to A&E. In total, I received 45 minutes of CPR while in the street, the ambulance and the Resus room. This was witnessed by my family who had arrived at the hospital long before I did.
At 1:04 pm the Consultant said that there was nothing further they could do and I was pronounced dead.
My family was ushered away in total shock to the family room and began to ring around relatives and friends, including work to inform them I had passed away.
However, the consultant returned some 20 or 30 minutes later to say they had found a pulse! He was not very optimistic and warned that they could not be sure how long my brain had been starved of oxygen and that even if I did survive I might have irreparable brain damage.
At 1:04 pm the Consultant said that there was nothing further they could do and I was pronounced dead.
It transpired that miraculously a young newly qualified nurse and health care assistant (HCA) had found a pulse while taking out all the tubes. He called the paramedic who had brought me in, who also felt a pulse, he immediately went to get the consultant to resume post-resuscitation care.
He later told me that he had to argue with the consultant to come back as he believed I just had agonal breathing which could not sustain life. Because this was all very unusual, John the paramedic visited me several times with his colleagues, he told me that he could feel a pulse both in my wrist and neck but it took him ten minutes to persuade the consultant to resume treatment as he didn’t think it was in my best interests.
My family then had to call people back with the news that I was alive, but I was still critically ill and there was only a small chance that I would survive, if I did I would most probably be brain damaged.
My battle was only just beginning but I was alive!
Alive
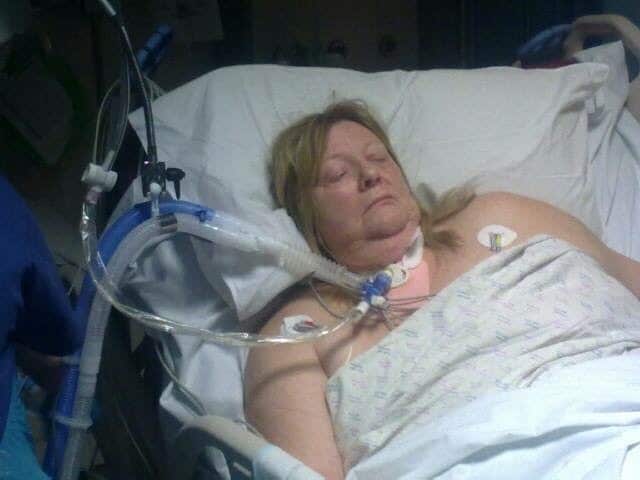
Fast forward to my recovery…
I was admitted to the CCU and was put into an induced coma and hypothermic state to try and reduce the brain damage that I might suffer, my family were warned that I may not survive and the outlook was grim.
When Doctors decided to try and wake me up, my family told me about the amazing care I had received and the story of what happened began to unfold. My first thoughts were that there must be something seriously wrong with my heart and I would need major heart surgery.
I had had quite a battle and things had looked rather grim
I could not easily ask questions or speak due to the tracheotomy I’d had done because I had become agitated and was not tolerating the tubes, which seems to be quite common. I could not tell anyone how I felt, I remember feeling terrified and in so much pain from the broken ribs I had sustained during CPR.
As I became more awake I was told what had happened to me it was all so very confusing and scary.
I had had quite a battle and things had looked rather grim.
I had two broken ribs from the CPR, which had nicked a blood vessel and caused my chest cavity to fill with blood collapsing my lung, resulting in a massive 5 litres blood loss. While still in a coma I had an emergency procedure to insert a chest drain, blood vessels would not stop bleeding so I was heavily sedated and given several blood transfusions and drugs to paralyse me to try and stop the bleeding, they even had to turn the airflow off the mattress.
Gradually I began to improve but I was so weak, and still reeling from the enormity of it all.
Air

The weeks passed and I became stronger and after about four weeks I was ready to get out of bed for the first time.
I remember clearly how wonderful it was when I first stood up, feeling the air all around me, but my legs didn’t feel my own, they were like jelly, I had to learn to walk again. At first, it didn’t seem that this would be possible, I was so weak I thought that I would never walk again properly but I did at first with the aid of a Zimmer frame, then with sticks. It was hard work but I was determined to get on my feet again.
After a month I was well enough to have the tracheotomy removed and I was transferred onto the cardiology ward. I had my first shower after four weeks and it was amazing and I began to feel almost human again. I was put on a monitor that showed that I was also having 6 to 8-second pauses where my heart would stop, usually at night.
I had an angiogram which came back normal so no furred up arteries, my echocardiogram was normal, so all good news, but still no reason for why I had suffered a cardiac arrest.
Doctors were reluctant to speculate but said it could have been something as simple as a chest infection. I was transferred to Stoke where I had an MRI, which again showed nothing except a couple of tiny blood clots caused by the bleed I had in my chest.
I spent 7 weeks in hospital and now I have an ICD fitted that will pace my heart should it need it and administer a shock if it ever goes into ventricular fibrillation again.
Home
I was discharged on 13th March and 3 months later, returned to work part-time, going full time after Christmas. Getting back to work and driving again was my main goal as I loved my job as Day opportunities coordinator and social inclusion lead for the local mental health trust.
Now 10 years on I can get on with my life and feel confident as I have my own internal cardiac defibrillator. I have no other problems with my heart and was discharged from the cardiologist after a year.
I did go and see the consultant who pronounced me dead to help provide closure for my family and the actions on that date were fully investigated. Several procedures had not been adhered to and I believe some resuscitation policies were amended to ensure it would not happen again to anyone else.
It was a hard slog getting back to fitness and overcoming the fatigue, which was sometimes overwhelming, but I can assure you that it does get better. As do the emotional feelings of guilt of putting my family through it, I’m sure it was much worse for them than for me.
But then there is this thing they call survivor’s guilt, the constant questioning, why did I survive when others didn’t?
There were several low ebbs when I didn’t think I was worthy and I did contemplate ending my life, even if only briefly.
Now I am just thankful to be alive.
Life

I love my life and will always be grateful for the care I received and especially to the nurse, HCA and paramedic who went the extra mile and advocated for me and made the consultant come back to me.
I owe my life to so many brilliant doctors, nurses, paramedics etc. and of course my family.
I do try to remain positive, I don’t always succeed.
My advice to anyone else going through this trauma is to just go with it, talk to others, there will always be good days and bad days but as time passes the good days outnumber the bad.
Be kind to yourself, keep challenging yourself to do a little more each day, but rest when you need to.
Become friends with your ICD if you have one.
It’s there to enable you not to disable yourself, he/she is like a good friend, is there when you need them.
Much Love
Sue Wyke
Ed: Sue is a very talented artist and has used it in her recovery, and here is some of her work…







What a fantastic, inspirational story Sue! So glad you’re around to share it! Embrace every second – I’m sure that you do.