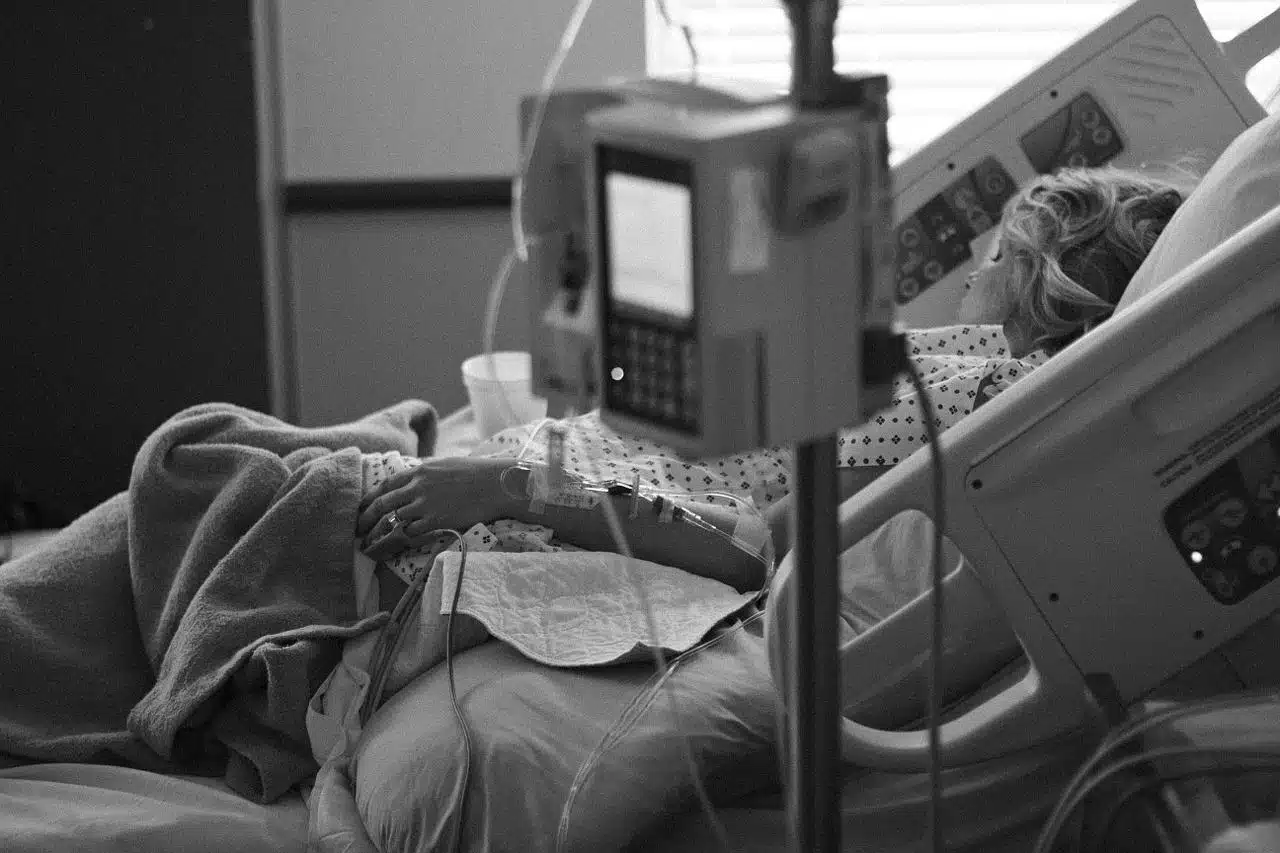
Experiencing a cardiac arrest and being admitted to an intensive care unit (ICU) can be an extremely daunting and overwhelming experience for the patient and loved ones. In this page, we aim to provide an in-depth guide to help patients and families understand what to expect during an ICU stay after surviving sudden cardiac arrest.
What is an Intensive Care Unit?
An ICU, also known as a critical care unit (CCU) or intensive therapy unit (ITU), is a specialised hospital ward that provides meticulous 24/7 monitoring and treatment for critically ill patients requiring intensive medical and nursing care.
ICUs are staffed by highly trained critical care specialists including intensivists, nurses, respiratory therapists, physical therapists, pharmacists, and more. The nurse to patient ratio is extremely high, usually 1:1 or 1:2, allowing for very close monitoring and care.
Why the ICU After Cardiac Arrest?
Sudden cardiac arrest halts blood flow to vital organs, most critically the brain, so admission to an ICU is crucial to maximize chances of survival and recovery.
Patients resuscitated after cardiac arrest are often placed in a medically induced coma and connected to a mechanical ventilator to ensure optimal oxygenation and prevent further brain injury. This makes it challenging to immediately discern the extent of neurological deficits incurred during the arrest.
Not All Cardiac Arrest Survivors Go to the ICU
While the ICU is standard for most resuscitated cardiac arrest patients, there are some scenarios where a patient may not be admitted to intensive care:
- If the cardiac arrest was very brief and full consciousness was rapidly regained, intensive monitoring may not be necessary.
- If serious comorbidities or advanced directives preclude aggressive ICU interventions, care may focus on comfort instead.
- Capacity constraints occasionally require prioritizing ICU beds for those most likely to benefit.
- In remote areas, urgent transport to a hospital with ICU services may not be feasible.
What to Expect in the Early ICU Phase
In the initial days after cardiac arrest, physicians employ various diagnostic tests to thoroughly evaluate brain function and look for signs of injury:
- Neurological reflex examination – assesses reflexes in limbs, responsiveness of pupils, and other markers of brain activity.
- Brain imaging – CT or MRI scans provide visualization of brain structure to identify any damage.
- Serial lab tests – track biomarkers, electrolyte levels, and other indicators of organ function.
- Continuous neurological monitoring – uses EEG and other tools to detect seizures and monitor brain activity.
For some patients, this watchful waiting phase can persist for over a week before a clearer prognosis emerges. The medical team takes a very judicious approach before making any definitive predictions about the extent of brain damage or chances for recovery.
Coping with ICU Delirium
The physical and emotional stress of an ICU stay after cardiac arrest can be profound. It is very common for patients to experience acute confusion, disorientation, and agitation, referred to as ICU delirium.
While delirium can be disturbing, it is usually temporary and begins to resolve as the brain heals. The comforting presence of loved ones can help reorient patients through bouts of delirium. Medical staff may also utilise strategies like adhering to day-night cycles or adjusting sedation levels to help stabilise cognition.
Other Common ICU Challenges
Along with delirium, other issues that frequently arise during ICU recovery include:
- Communication difficulties – Intubation injuries can initially make speaking and swallowing difficult after extubation. Assistive communication devices and speech therapy aid in regaining function.
- Weakness – Prolonged ICU stays lead to severe muscle deconditioning. Physical and occupational therapy help rebuild strength. Mobilization occurs as soon as medically feasible.
- Anxiety, depression – The trauma, uncertainty, and altered cognition provoke distress. Emotional support from staff and family is key. Psychiatric medications or counselling may also help.
- Sleep disruptions – ICU environment hinders quality sleep. Staff minimize nighttime interruptions and noise/light as able. Melatonin or sleep aids can also be useful.
With perseverant rehabilitation and support, most physical and psychological symptoms substantially resolve over the course of recovery.
Predicting Outcomes After Cardiac Arrest

Prognostication after cardiac arrest is extremely complex, given the many obscure variables impacting outcomes. There are no 100% accurate predictive models. However, physicians utilise multimodal assessments – neurological tests, imaging, lab work, and treatment response – to provide the most accurate estimate possible.
Specialised scoring systems like the Glasgow Coma Scale and Cerebral Performance Category help standardise assessments of neurological recovery. However, prognoses are determined based on a holistic evaluation rather than any single metric.
Doctors convey prognoses cautiously and compassionately, avoiding premature predictions. Expect ongoing dialogue and updates from the care team as the clinical trajectory evolves in the ICU.
In Episode #48 of our podcast, Life After Cardiac Arrest, we interview consultant neurologist Professor Tobias Cronberg from Lund University in Sweden. The discussion revolves around predicting patients’ post-cardiac arrest progress, specifically focusing on prognostication. Professor Cronberg shares insights into the tools, techniques, and decision-making processes involved in assessing potential outcomes.
https://feeds.acast.com/public/shows/5cd98d1c383108353c6451b5Visiting Loved Ones in the ICU
Despite the complexities of critical care, the overarching focus remains restoring patients to optimal functioning. The involvement of loved ones is a crucial element. Family members should receive education on what to expect in the ICU and how best to participate in the healing process:
- Ask questions – Seek explanations from care staff on treatments, changes in condition, expected outcomes.
- Participate in rounds – Attend multidisciplinary rounds to stay updated on progress and care goals.
- Provide comfort – Your familiar voice and touch help ground patients amid the chaos.
- Aid in orientation – Gently reorient your loved one by sharing who is there and where he/she is.
- Advocate needs – Make staff aware of any concerns about pain, anxiety, confusion that need addressing.
While an ICU stay is daunting, patients and families are never alone. With compassionate support from caregivers and loved ones, survivors can progress along the recovery continuum – navigating the twists and turns of the ICU journey to emerge revitalised ultimately.
More Help
The primary UK charity for patients staying in the intensive care unit is ICU Steps. They have plenty of resources on their website, and support groups dotted around the country.


On the Road to Recovery
The East Suffolk and North Essex NHS Foundation Trust have produced an excellent video showcasing the critical care patients receive during their recovery journey.
Further Reading
Unexpected recoveries from long-term coma after cardiac arrest
Clinical predictive models of SCA – Survey and analysis
Miracle2 – Risk score for early prediction – study
Miracle2 – Risk score for early prediction – review
NHS Intensive Care – Overview